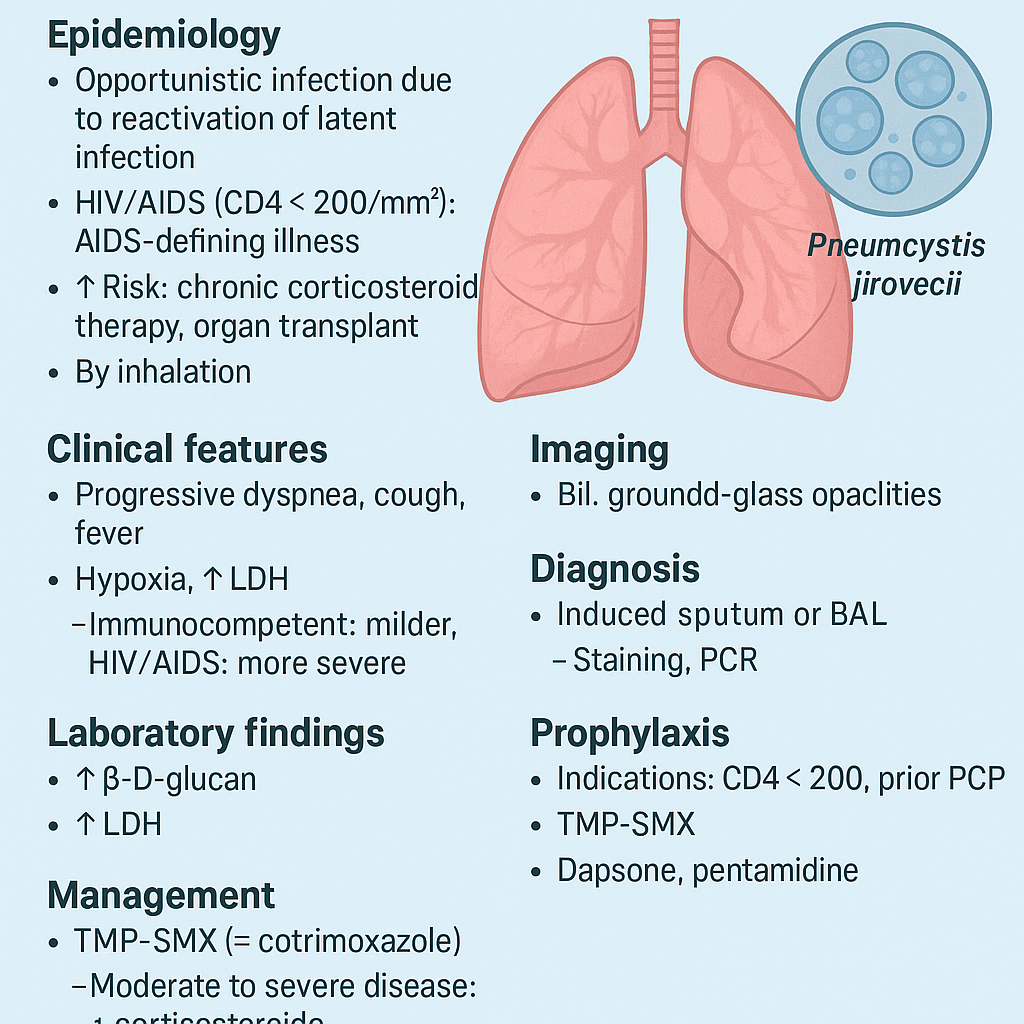
pneumocystis jirovecii
---
# **📘 25 CASE SCENARIOS — PNEUMOCYSTIS JIROVECII (PCP)**
---
## **CASE 1 — Classic HIV PCP**
A 32-year-old male with newly diagnosed HIV (CD4 = 84) presents with **progressive dyspnea × 3 weeks**, dry cough, fever.
SpO₂ drops from 94% to 82% on minimal exertion.
CXR: **Bilateral diffuse ground-glass opacities**.
LDH: 560 U/L.
ABG: PaO₂ 60 mmHg.
**Diagnosis:** Moderate–severe PCP
**Management:** IV TMP–SMX + prednisone taper.
---
## **CASE 2 — Sudden deterioration**
A patient on day 4 of TMP–SMX for PCP suddenly develops acute pleuritic pain and hypoxia.
CXR: **Large right pneumothorax**.
**Complication:** PCP-related pneumothorax (due to subpleural cyst rupture).
**Management:** Chest tube + continue PCP treatment.
---
## **CASE 3 — Non-HIV, rapid onset**
A 60-year-old man on **prednisone 40 mg/day for 2 months** (interstitial lung disease) develops acute dyspnea × 3 days.
Very hypoxic.
CXR: diffuse interstitial infiltrates.
**Diagnosis:** Non-HIV PCP
**Management:** IV TMP–SMX; early steroids (PaO₂ <70).
---
## **CASE 4 — HIV patient on ART default**
A 28-year-old defaulted ART for 1 year.
Now presents with weight loss + fever + cough.
CD4 = 36.
β-D-glucan positive.
**Diagnosis:** PCP
**Management:** TMP–SMX; start ART after **2 weeks** (to avoid IRIS).
---
## **CASE 5 — Prophylaxis failure**
A 44-year-old HIV patient on **dapsone prophylaxis** develops PCP.
G6PD was never checked.
**Diagnosis:** Breakthrough PCP (dapsone failure due to improper absorption or resistance).
**Management:** Switch to TMP–SMX; check G6PD.
---
## **CASE 6 — Transplant patient**
A kidney-transplant recipient on tacrolimus + prednisone presents with progressive dyspnea, dry cough, fever.
CT: **ground-glass infiltrates**.
**Diagnosis:** PCP in transplant recipient
**Management:** IV TMP–SMX + careful renal dosing + steroids.
---
## **CASE 7 — Cancer chemotherapy**
A 52-year-old woman receiving rituximab for lymphoma presents with fever, tachypnea, dry cough × 5 days.
HRCT: diffuse GGO; LDH elevated.
BAL PCR positive.
**Management:** TMP–SMX + prednisone.
---
## **CASE 8 — Post-COVID immune suppression**
A man received high-dose steroids for COVID ARDS.
Now, 6 weeks later: fever, breathlessness.
CT: ground-glass infiltrates.
**Diagnosis:** Steroid-induced PCP
**Management:** TMP–SMX ± steroids.
---
## **CASE 9 — Mild PCP**
A 33-year-old HIV+ woman, CD4 = 170, has mild dry cough and fever.
PaO₂ = 76 mmHg.
**Management:** Oral TMP–SMX (mild); no steroids.
---
## **CASE 10 — Severe PCP with respiratory failure**
HIV+ man arrives in ED with RR 40/min, cyanosis.
PaO₂ = 48 mmHg.
**Diagnosis:** Severe PCP
**Management:** ICU care + IV TMP–SMX + IV methylprednisolone.
---
## **CASE 11 — Patient allergic to sulfa**
HIV+ woman with known SJS to sulfa drugs presents with PCP.
**Management:**
* Clindamycin + primaquine
* Or IV pentamidine if severe
* Test G6PD before primaquine.
---
## **CASE 12 — PCP in poorly nourished patient**
A 50-year-old alcoholic with severe malnutrition develops dyspnea × 10 days.
BAL positive.
**Management:** TMP–SMX; screen for electrolyte disturbances.
---
## **CASE 13 — β-D-glucan positive but CXR normal**
Early PCP: LDH high, β-D-glucan positive, but normal X-ray.
HRCT shows patchy ground-glass changes.
**Diagnosis:** Early PCP
**Management:** TMP–SMX.
---
## **CASE 14 — PCP in pregnancy**
HIV+ pregnant woman with CD4 = 90 presents with worsening breathlessness.
CT avoided; X-ray shows diffuse infiltrates.
**Management:** TMP–SMX (benefits outweigh risks); steroids if indicated; folinic acid.
---
## **CASE 15 — Relapse after stopping prophylaxis early**
HIV patient stopped TMP–SMX prophylaxis when CD4 became 210 for only 6 weeks.
Now presents with PCP.
**Cause:** Prophylaxis was stopped too early.
**Management:** Full treatment + restart prophylaxis until CD4 >200 for **≥3 months**.
---
## **CASE 16 — Hyperkalemia due to therapy**
A patient on high-dose TMP–SMX for PCP develops K⁺ = 6.1.
**Cause:** TMP inhibits renal potassium excretion.
**Management:** Treat hyperkalemia; adjust TMP–SMX dose.
---
## **CASE 17 — AKI during therapy**
Creatinine rises to 2.4 mg/dL on TMP–SMX.
**Management:**
* Dose adjust
* Monitor electrolytes
* Ensure hydration
* Consider alternative if worsening.
---
## **CASE 18 — PCP vs CMV pneumonia confusion**
Transplant patient has fever and diffuse infiltrates.
PCP stains negative; CMV PCR very high.
**Diagnosis:** CMV pneumonia (PCP mimic).
**Management:** Ganciclovir.
---
## **CASE 19 — PCP in patient on TNF-α inhibitor**
A patient on infliximab for rheumatoid arthritis develops fever, progressive breathlessness.
CT: interstitial GGO.
**Diagnosis:** Immunosuppression-related PCP
**Management:** TMP–SMX.
---
## **CASE 20 — PCP with severe hyponatremia**
A patient develops Na = 121 due to TMP–SMX + SIADH-like effect.
**Management:** Correct sodium + continue treatment with caution.
---
## **CASE 21 — PCP + Pneumothorax + ARDS overlap**
Severely ill PCP patient on ventilator suddenly has worsening hypoxia.
CXR: bilateral infiltrates + small pneumothorax.
**Management:**
* Ventilation with low tidal volume
* Chest tube if needed
* Continue PCP therapy.
---
## **CASE 22 — PCP in untreated HIV found incidentally**
A homeless patient with chronic cough is brought in.
CXR done for TB screening shows diffuse opacities.
BAL reveals PCP.
**Management:** TMP–SMX + ART initiation after 2 weeks.
---
## **CASE 23 — PCP in obesity-hypoventilation syndrome**
Obese immunosuppressed patient presents with confusion and dyspnea.
ABG: Severe hypoxemia + hypercapnia.
**Management:**
* NIV/CPAP
* TMP–SMX
* Steroids
* Slow oxygen escalation to avoid CO₂ retention.
---
## **CASE 24 — PCP in patient with hematologic malignancy**
AML patient receiving chemotherapy becomes febrile and dyspneic.
CT: diffuse bilateral GGO.
BAL PCR: positive for *P. jirovecii*.
**Management:** IV TMP–SMX; consider pentamidine if neutropenia.
---
## **CASE 25 — PCP diagnosed only on HRCT**
CXR normal.
HRCT: classic ground-glass with septal thickening (“crazy-paving”).
BAL unavailable.
**Diagnosis:** Radiologic PCP
**Management:** TMP–SMX.
---
Hard Case-Based MCQs – PCP Pneumonia
Focus: risk stratification, drug regimens, toxicities, and tricky differentials in immunocompromised patients.