Premature Rupture of Membranes PROM – Causes Diagnosis Management and Complications
Below is a **complete, SEO-friendly, exam-oriented, single-place medical reference** on **Premature Rupture of Membranes (PROM)**, structured with clear **H1–H4 headings**, rich keywords, and clinically accurate content suitable for **medical students, clinicians, and health websites**.
---
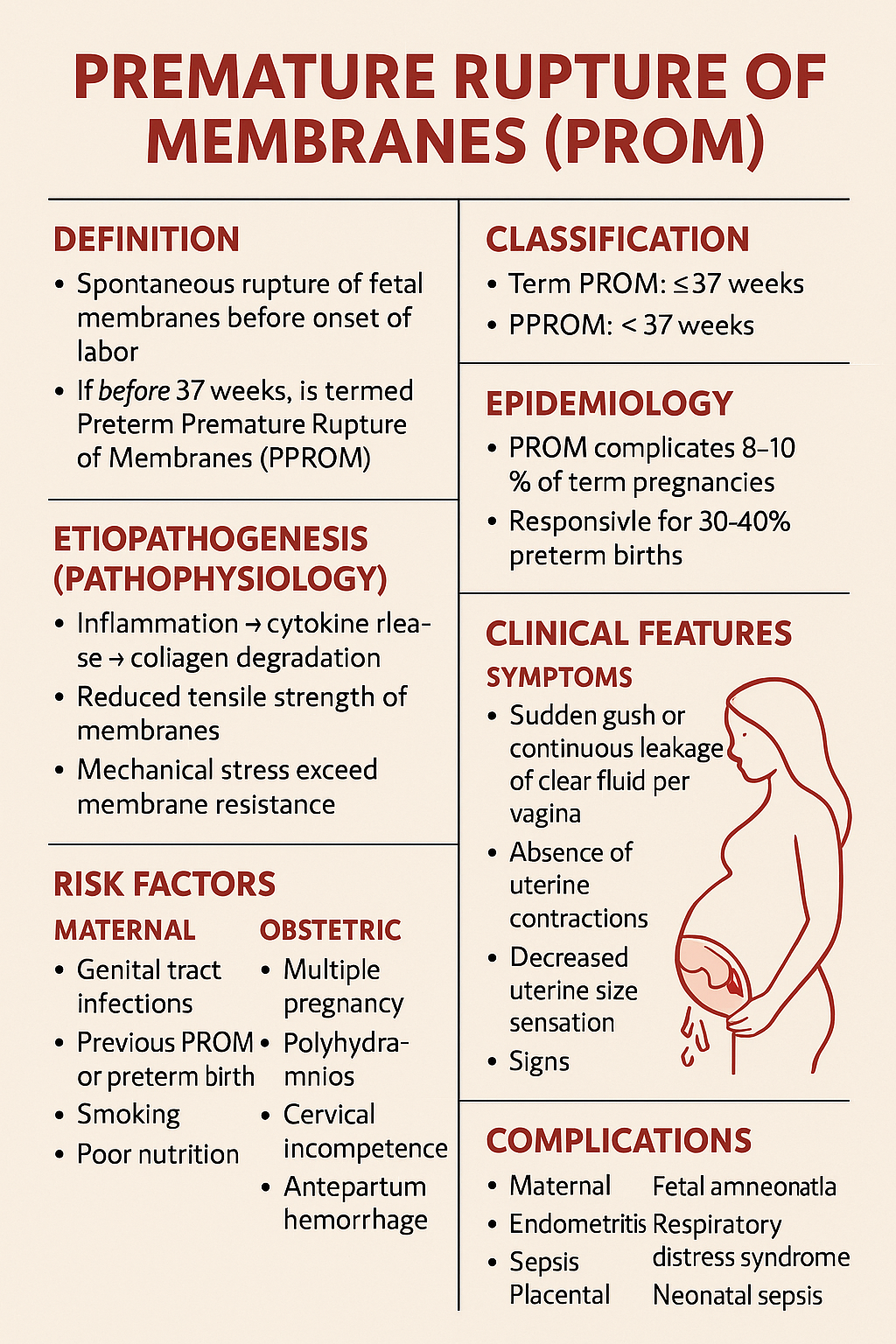
# **Premature Rupture of Membranes (PROM)**
## **Definition**
**Premature Rupture of Membranes (PROM)** is defined as **spontaneous rupture of the fetal membranes before the onset of labor**, irrespective of gestational age.
* If it occurs **before 37 completed weeks**, it is termed **Preterm Premature Rupture of Membranes (PPROM)**.
---
## **Classification**
### **1. Based on Gestational Age**
* **Term PROM**: ≥ 37 weeks
* **PPROM**: < 37 weeks
### **2. Based on Duration**
* **Recent PROM**: < 18 hours
* **Prolonged PROM**: ≥ 18 hours (↑ risk of infection)
---
## **Epidemiology**
* PROM complicates **8–10% of term pregnancies**
* PPROM accounts for **2–3% of all pregnancies**
* Responsible for **30–40% of preterm births**
---
## **Etiopathogenesis (Pathophysiology)**
### **Normal Membrane Integrity**
* Maintained by **collagen, elastin, and extracellular matrix**
* Balance between **matrix synthesis and degradation**
### **Mechanisms Leading to PROM**
* **Inflammation → cytokine release → collagen degradation**
* **Reduced tensile strength of membranes**
* **Mechanical stress exceeding membrane resistance**
---
## **Risk Factors**
### **Maternal Factors**
* Genital tract infections (BV, UTI, STIs)
* Previous PROM or preterm birth
* Smoking
* Poor nutrition
* Low socioeconomic status
### **Obstetric Factors**
* Multiple pregnancy
* Polyhydramnios
* Cervical incompetence
* Antepartum hemorrhage
### **Iatrogenic Factors**
* Amniocentesis
* Cervical procedures
---
## **Clinical Features**
### **Symptoms**
* Sudden **gush or continuous leakage of clear fluid per vagina**
* Absence of uterine contractions initially
* Decreased uterine size sensation
### **Signs**
* Pooling of liquor in posterior fornix
* Wet perineum
* Reduced amniotic fluid volume
---
## **Diagnosis**
### **History**
* Timing, amount, color, and odor of fluid
* Associated fever, pain, reduced fetal movements
### **Physical Examination**
* **Sterile speculum examination (preferred)**
* Avoid digital vaginal examination unless in labor
---
### **Confirmatory Tests**
#### **1. Bedside Tests**
* **Nitrazine test**: Alkaline pH (false positives possible)
* **Fern test**: Crystallization pattern on microscopy
#### **2. Biochemical Tests**
* PAMG-1 (AmniSure)
* IGFBP-1 (Actim PROM)
#### **3. Ultrasound**
* Reduced Amniotic Fluid Index (AFI)
* Assessment of fetal growth and presentation
---
## **Differential Diagnosis**
* Urinary incontinence
* Physiological vaginal discharge
* Seminal fluid
* Vaginal infections
---
## **Complications**
### **Maternal**
* Chorioamnionitis
* Endometritis
* Sepsis
* Placental abruption
### **Fetal and Neonatal**
* Prematurity
* Respiratory distress syndrome
* Neonatal sepsis
* Umbilical cord prolapse
* Pulmonary hypoplasia (early PPROM)
---
## **Management of PROM**
Management depends on **gestational age**, **infection status**, and **fetal condition**.
---
## **Management at Term PROM (≥ 37 Weeks)**
### **Principles**
* Aim for **delivery**
* Reduce infection risk
### **Management**
* Induction of labor within **12–24 hours**
* Oxytocin preferred
* Prophylactic antibiotics if GBS positive
---
## **Management of PPROM (< 37 Weeks)**
### **General Principles**
* Balance between **prematurity risks** and **infection risks**
* Expectant management if stable
---
### **Stepwise Management**
#### **1. Hospitalization and Monitoring**
* Maternal vitals, fetal heart rate
* Signs of infection
#### **2. Antibiotic Therapy**
**Indication**: Prolong latency, reduce infection
**Standard Regimen**
* Ampicillin IV → Amoxicillin oral
* Erythromycin / Azithromycin
**Benefits**
* ↓ Chorioamnionitis
* ↓ Neonatal sepsis
* ↑ Latency period
---
#### **3. Corticosteroids**
**Indication**: 24–34 weeks
**Drugs**
* Betamethasone 12 mg IM × 2 doses (24 hours apart)
**Benefits**
* ↓ RDS
* ↓ IVH
* ↓ NEC
---
#### **4. Tocolysis**
* **Not routinely recommended**
* Short-term use only to complete steroid course
---
#### **5. Magnesium Sulfate**
**Indication**: < 32 weeks
**Purpose**: Fetal neuroprotection
---
### **Indications for Immediate Delivery**
* Clinical chorioamnionitis
* Non-reassuring fetal status
* Placental abruption
* Advanced labor
* Severe oligohydramnios with distress
---
## **Prevention**
* Screening and treatment of genital infections
* Smoking cessation
* Cervical cerclage in indicated cases
* Adequate antenatal care
---
## **Prognosis**
* **Term PROM**: Excellent with timely delivery
* **PPROM**: Depends on gestational age and infection
* Neonatal outcome improves significantly after **32–34 weeks**
---
## **Key Exam Points**
* Avoid digital vaginal examination in PROM
* Antibiotics increase latency in PPROM
* Corticosteroids between 24–34 weeks
* Infection = indication for delivery at any gestation
---
## **SEO Keywords (Comma-Separated)**
premature rupture of membranes, prom pregnancy, pprom obstetrics, prom diagnosis management, preterm premature rupture membranes, prom complications, amniotic fluid leakage pregnancy, chorioamnionitis prom, prom treatment guidelines, pprom antibiotics steroids
---
If you want, I can next:
* Generate **SEO-optimized title and meta description**
* Create **25 hard case-based MCQs (HTML CSS JS in one file)**
* Generate **FAQ schema for SEO**
* Provide **image prompts or medical diagrams**